How Often Should You Get Your Heart Checked?
You probably know your heart beats around 100,000 times a day—but do you know if it’s beating as healthily as it should? Many people assume they’re fine… until they’re not. So, how often should you get your heart checked, really? The answer isn’t as simple as a number, and what you’ll discover might change the way you think about your next appointment.
TL;DR
Heart screening frequency depends on age, risk factors, family history, lifestyle, and symptoms—not just a specific number. Screening can begin in childhood for specific cases, with baseline evaluations in young adulthood and intensified monitoring after 40 or earlier for high-risk individuals. Those with genetic risk, chronic conditions, or unhealthy habits may need earlier and more frequent testing. Prevention, regular monitoring, and healthy lifestyle choices are key to reducing cardiovascular risk.
Book a cardiac consultation in Brooklyn now
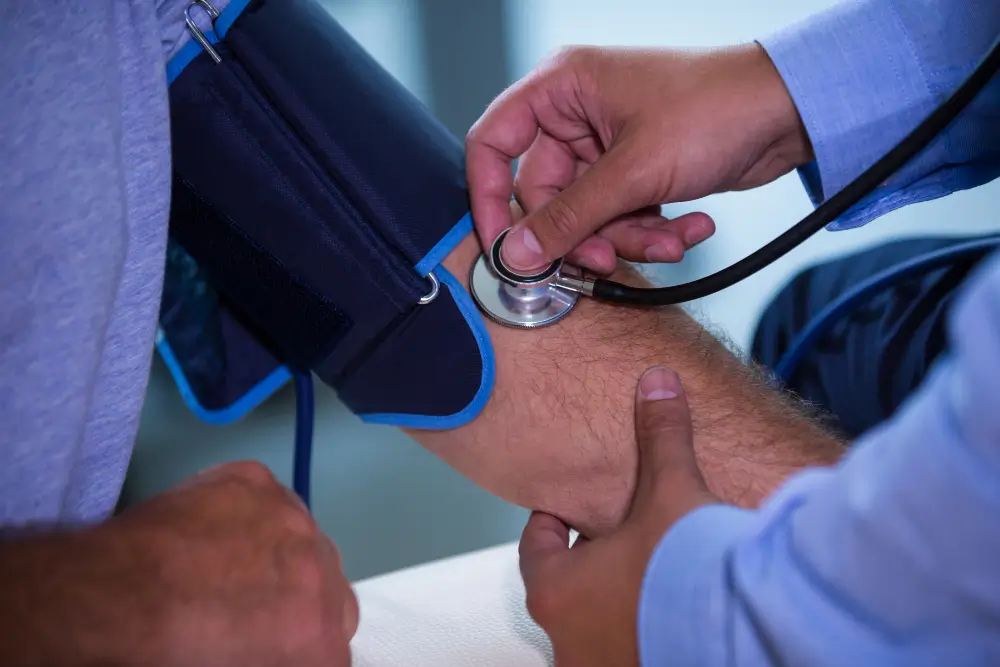
What Age Should Heart Screenings Begin?
Age and personal risk factors determine when heart screenings should start. Cardiac screening begins at birth to detect congenital heart conditions and allow early intervention. Cholesterol testing is recommended between ages 9 and 11 and may be done earlier if there is family history or elevated risk to identify lipid abnormalities early.
Young adults should have an initial evaluation if they have no symptoms or relevant medical history. In general, laboratory testing is recommended every 3 years, an electrocardiogram every 5 years, and blood pressure checks every 2 years. These evaluations establish a cardiovascular baseline.
After age 35–40, follow-up should become more frequent, especially with a family history of heart disease, and may include consultation with a cardiology specialist. Individuals with obesity, diabetes, hypertension, or family history should begin screening earlier or undergo more frequent evaluations. Final screening intervals should always be determined based on individual risk profile and medical guidance.
General Age Guidelines for Initial Heart Screenings
Guidelines for initial heart screenings vary by age and individual risk level. There is no single universal starting point, as family history, smoking, hypertension, and metabolic conditions directly influence timing.
| Age Group | Main Recommendation | Considerations |
| 6–16 years | Evaluation for athletes | Based on physical activity level |
| 40–50 years | Begin preventive checkups | Assess risk factors |
| 65+ years | ECG and biomarkers | Especially before surgeries |
| Any age with symptoms | Immediate evaluation | Chest pain, shortness of breath, dizziness, palpitations |
Initial heart tests should be adapted to age, risk factors, and symptoms. Some evaluations begin at specific life stages, but individualized assessment remains essential. Identifying risks, recognizing warning signs, and completing basic testing create a clear foundation for cardiovascular care.
Early Screening for High-Risk Individuals
Early screening in individuals at high cardiovascular risk focuses on regular checkups designed to identify abnormalities before symptoms appear. It is especially recommended for those with family history, smoking history, diabetes, obesity, or chronic disease, as it allows timely intervention and reduces the likelihood of serious events.
Components of Early Screening
- Lipid profile: Measures total cholesterol, LDL, and HDL; recommended at least every 4–6 years starting at age 20, more frequently if risk factors are present.
- Blood pressure: Regular monitoring to detect hypertension.
- Blood glucose: Evaluates for diabetes.
- High-sensitivity C-reactive protein: Indicates inflammation associated with cardiovascular risk.
- Coronary calcium score (CT): Five-minute scan measuring calcium buildup in coronary arteries.
- Electrocardiogram (ECG): Assesses electrical activity and heart structure.
- AI-assisted ECG: Detects low ejection fraction and hypertrophic cardiomyopathy.
- Risk calculators (Framingham, SCORE, ECVAA): Estimate risk based on age, sex, smoking, and family history.
- Automatic high-risk category: Individuals with type 2 diabetes, chronic kidney disease (filtration <60), or inflammatory diseases.
Early detection in high-risk individuals supports intensive lifestyle modifications and early lipid-lowering therapy. Identifying risk factors and completing targeted evaluations helps prevent cardiovascular complications before symptoms develop.
Family History and Genetic Considerations
Family history of heart disease significantly increases cardiovascular risk, especially when a parent or sibling was diagnosed before age 55 in men or 65 in women. This risk may result from genetic mutations or shared lifestyle patterns, making early and consistent monitoring essential.
Genetic and Family Risk Factors
- First-degree relatives diagnosed 10–20 years earlier than average age = high risk
- Both parents with early heart disease = up to 50% increased risk
- Genetic cardiomyopathies and channelopathies = 50% transmission probability
- Familial hypercholesterolemia and type 2 diabetes = strong genetic component
- Increased surveillance recommended with family history of sudden death or syncope
When significant family history exists, screening should not be delayed. Identifying risk, completing regular testing, and adopting preventive measures reduce the likelihood of complications before symptoms appear.
Lifestyle Factors That Influence Screening Age
Lifestyle habits directly influence the age at which heart screening should begin. Smoking, poor diet, physical inactivity, obesity, chronic stress, and alcohol consumption accelerate arterial damage and may require evaluation before 40–50 years of age.
Main Lifestyle Factors
- Smoking: Damages arterial walls and increases need for early screening
- High-fat, high-salt diet plus abdominal obesity: Contribute to hypertension and diabetes
- Physical inactivity: Raises metabolic and cardiovascular risk
- Chronic stress: Increases blood pressure and unhealthy behaviors
- Alcohol: May cause arrhythmias and heart muscle damage
- Early monitoring recommended: Blood pressure, cholesterol, and glucose
When these factors are present, cardiovascular risk appears earlier than expected. Starting screening sooner allows early detection and lowers the chance of future complications.
Recommendations From Primary Care Providers
Primary care providers recommend a preventive, lifestyle-focused approach to heart health. This includes at least 150 minutes of weekly exercise, maintaining a healthy weight, reducing salt intake, and following a diet rich in fruits, vegetables, and fiber. They also emphasize regular monitoring of blood pressure, cholesterol, and blood sugar while avoiding tobacco use.
Daily physical activity of 30–60 minutes, combining aerobic and strength exercises, is encouraged. Household activities and gardening also count.
A balanced diet centered on fresh foods is recommended, limiting fast food, processed products, sugary beverages, and processed meats. Avoiding smoking and secondhand smoke, managing stress, and prioritizing restorative sleep are especially beneficial for individuals with family history of heart disease, diabetes, or hypertension.
Referral to a specialist should be considered if chest discomfort, shortness of breath, or palpitations occur, or if blood pressure or cholesterol are difficult to control. Strong family history or abnormal results on basic tests such as ECG or laboratory studies warrant further evaluation. Early detection and consistent risk management provide the strongest defense against cardiovascular complications.
Key Takeaways
- Heart check frequency depends on individual risk, not just age: There is no single rule for when to get screened. Age, lifestyle, family history, symptoms, and chronic conditions all influence timing and frequency. Prevention and regular monitoring are essential to reduce cardiovascular risk.
- Screening can begin early and increases with age or risk: Heart evaluations may start at birth for congenital conditions and include cholesterol testing in childhood. Young adults establish a baseline, while monitoring typically intensifies after 40. Those with risk factors may need earlier and more frequent assessments.
- High-risk individuals require proactive and specialized screening: People with diabetes, obesity, smoking history, kidney disease, or strong family history benefit from earlier testing. Monitoring may include cholesterol panels, blood pressure, glucose, ECGs, coronary calcium scans, and risk calculators. Early detection allows timely lifestyle changes and preventive treatment.
- Family history and genetics significantly impact screening needs: Early heart disease in first-degree relatives increases personal risk, especially if it occurs well before average age. Certain genetic heart conditions and inherited disorders raise risk further. Consistent monitoring and preventive action are critical in these cases.
- Lifestyle choices directly influence when screening should begin: Smoking, poor diet, inactivity, stress, obesity, and alcohol use accelerate arterial damage. These factors can shift screening to earlier ages. Primary care providers emphasize exercise, healthy eating, risk monitoring, and avoiding tobacco as the foundation of heart health.
FAQs
Should you get your heart checked regularly?
Yes. Heart screenings should begin around age 20 and continue every 2–4 years in healthy young adults without symptoms or family history. If you are under 40 with no risk factors, a check every 3–5 years may be sufficient. Regular monitoring helps detect early changes in blood pressure, cholesterol, and overall cardiovascular health.
What are four signs your heart is in trouble?
Key warning signs include chest discomfort (pressure or squeezing), shortness of breath, unusual fatigue or weakness, and irregular or pounding heartbeats (palpitations). These symptoms may be accompanied by dizziness, jaw pain, sweating, or swollen legs. Because they can signal serious conditions, prompt medical evaluation is essential.
How often should I see my cardiologist?
The frequency depends on your risk profile. Individuals without risk factors may need a visit every few years, while those with high blood pressure, diabetes, or family history often require annual or more frequent follow-ups. In more serious conditions, such as heart failure, visits may be scheduled every few months according to medical guidance.
How often should you have a healthy heart check?
For adults under 40 with no symptoms or family history, a heart check is generally recommended every 3–5 years. These visits typically include blood pressure measurement, cholesterol testing, and a general health assessment. The schedule should always be adjusted based on individual risk factors and clinical findings.
Sources
- Davis, W. (2005). What Does My Heart Scan Show?.
https://www.cureality.com/library/What%20Does%20My%20Heart%20Scan%20Show%20v042805.pdf
- Mullainathan, S., & Obermeyer, Z. (2019). Who is tested for heart attack and who should be: Predicting patient risk and physician error (pp. 1-48). Cambridge, MA, USA: National Bureau of Economic Research.
https://www.nber.org/system/files/working_papers/w26168/revisions/w26168.rev0.pdf?mod=article_inline
